Laser Dentistry
- Home
- Treatments
- Laser Dentistry
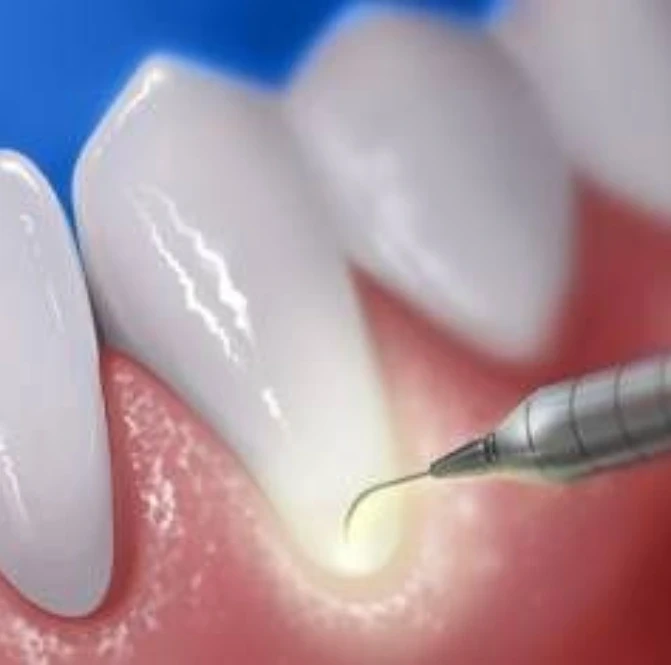
What is laser dentistry? It is the use of concentrated light energy to perform dental procedures with far greater precision and comfort than a drill or scalpel. At Vitrin Clinic, we use state of the art laser dentistry technology across a wide range of soft tissue, hard tissue, and cosmetic procedures replacing drills with a precise beam of light that cuts, sterilises, and heals in one motion. Less pain. Less bleeding. Less time in the chair.
Treatment Process
A clear step-by-step overview of how the treatment is planned and performed, from the initial consultation to the final results, ensuring comfort, safety, and predictable outcomes.
01
Consultation & Assessment
Your dentist examines the area of concern using digital X-rays or intraoral imaging where needed and confirms whether laser treatment is the optimal approach for your specific case. Not every procedure is best served by laser; we recommend it only where it offers a genuine clinical advantage.
02
Protective Preparation
You'll be given protective eyewear before treatment begins a standard requirement for all laser procedures. Anaesthetic gel or local anaesthesia is applied if needed, though many laser procedures require neither.
03
Laser Treatment
The laser handpiece is positioned precisely over the treatment site. You may feel warmth or mild pressure, but for most procedures there is no pain. The laser works quickly soft tissue procedures are often complete within 15–30 minutes, with no drill vibration or noise throughout.
04
Immediate Post-Treatment
The laser-treated area will appear slightly whitened initially a normal reaction. Bleeding is minimal to absent for soft tissue cases. Most patients can eat, speak, and return to normal activity the same day, particularly for gum-based procedures.
05
Aftercare & Follow Up
We provide clear aftercare instructions tailored to your specific procedure. For gum treatments, this typically involves a gentle saltwater rinse routine and a soft diet for 2–3 days. A follow up review is scheduled to confirm healing and assess results.
What Is Laser Dentistry?
Laser dentistry encompasses the use of focused light energy to perform a wide range of dental procedures on soft tissue, hard tissue, and bone replacing or supplementing conventional mechanical instruments in specific clinical applications.
The term LASER is an acronym for Light Amplification by Stimulated Emission of Radiation.
In clinical dentistry, different laser wavelengths are absorbed differently by water, haemoglobin, and dental tissue meaning that specific laser types are suited to specific tissue targets and clinical objectives.
Lasers have been used in dentistry since the 1960s, with clinical applications expanding significantly from the 1990s onward as the evidence base for their safety and efficacy developed.
A 2025 narrative review from NIH/PMC covering 67 articles published between 2018 and 2023 confirmed that laser technology has reached an advanced stage of clinical development across periodontics, implantology, endodontics, soft tissue surgery, and photobiomodulation, with measurable benefits over conventional approaches in specific, evidence-defined applications.
At Vitrin Clinic, lasers are used where the clinical evidence supports their use as the most appropriate tool for the procedure not as a marketing claim applied universally.
The right laser wavelength and energy parameters are selected based on the tissue target and the clinical objective.
Lasers are one precision instrument in a clinical toolkit; they are used where they produce measurably better outcomes, and conventional instruments are used where they do not.
Laser-Assisted Procedures vs. Conventional Techniques
The following comparison reflects the evidence-based clinical differences between laser-assisted and conventional approaches across the primary dental procedures where laser use is supported by peer-reviewed research.
Laser treatment is not universally superior its advantages are procedure-specific and patient-specific.
Clinical Parameter | Laser-Assisted Procedure | Conventional Technique |
|---|---|---|
Intraoperative Bleeding | Significantly reduced immediate haemostasis through vessel coagulation | Bleeding managed with pressure, sutures, or electrocautery |
Post-Operative Pain | Measurably lower confirmed in systematic review meta-analysis (TMDU, 2020) | Managed with analgesics higher pain scores reported vs. laser groups |
Wound Healing Rate | Faster epithelialisation PBM accelerates cellular repair processes (PMC11531730, 2024) | Standard healing timeline dependent on tissue and patient factors |
Sutures Required | Often not required for soft tissue coagulation seals wound margins | Usually required for soft tissue incisions |
Anaesthesia Required | Reduced or eliminated in many soft tissue procedures | Local anaesthesia typically required for all surgical procedures |
Bactericidal Effect | Yes laser irradiation reduces bacterial load at treatment site | Mechanical debridement only bacteria may persist in inaccessible areas |
Patient Anxiety | Lower reduced drill noise, vibration, and pain association | Higher for drill-averse patients sound and vibration are reported anxiety triggers |
Applicable to All Procedures | No specific indications; not universally superior to conventional | Yes gold standard for many procedures remains conventional approach |
Learning Curve | Requires specific training inadequate learning curve leads to failures (PRISMA review, 2023) | Established technique broad clinical training base |
Compiled from: Tokyo Medical and Dental University — Laser-Assisted Pain Control After Periodontal Therapy, PMC7498060 · Manav Rachna Dental College — LLLT Efficacy in Oral Wound Healing, PMC11531730, 2024 · NIH/PMC — Therapeutic and Adverse Effects of Lasers in Dentistry: Systematic Review, MDPI Photonics, 2023 · NIH/PMC — Laser Technology in Dentistry: Clinical Applications to Future Innovations, PMC11674728, 2025.
Why Clinical Approach Matters
Laser dentistry is a field where the clinical approach matters more than the presence of the equipment.
A laser device in a clinic does not guarantee better outcomes the wavelength must be matched to the tissue target, the energy parameters must be set correctly for the clinical objective, and the clinician must have the training and experience to operate the system safely and effectively.
A systematic review published in MDPI Photonics following PRISMA guidelines using PubMed, Scopus, and Web of Science explicitly identified inadequate learning curve and non-targeted laser selection based on clinical need as the primary causes of treatment failures in laser dentistry.
The technology does not substitute for clinical judgement; it extends it.
The distinction between laser wavelengths is clinically critical.
Diode lasers operate in the near-infrared spectrum and are absorbed by haemoglobin and melanin making them ideal for soft tissue incision, haemostasis, and periodontal pocket disinfection, but ineffective on hard tissue. Erbium lasers (Er:YAG and Er,Cr:YSGG) are absorbed by water making them effective on enamel, dentine, and bone, as well as soft tissue, but requiring different energy parameters and technique.
Using the wrong wavelength for a clinical application produces inadequate results and risks collateral tissue damage.
Photobiomodulation the non-ablative, biostimulatory application of laser energy is the area of fastest-growing clinical evidence in dental laser research. Its mechanism is well-characterised at the cellular level: activation of mitochondrial cytochrome c oxidase increases ATP production and triggers a cascade of anti-inflammatory and pro-healing cellular events. At Vitrin Clinic, PBM is applied as a clinical adjunct where the evidence supports measurable benefit including post-surgical wound healing, pain management following periodontal therapy, and recovery following soft tissue surgery.
What the research shows
Significant | 100% | Critical |
|---|---|---|
Reduction in postoperative pain following laser-assisted periodontal therapy versus conventional treatment alone confirmed in a systematic review and meta-analysis of randomised controlled trials from Tokyo Medical and Dental University (TMDU), one of Japan's leading dental research institutions. | Of 14 studies included in a 2024 systematic review found a substantial difference between laser and control groups in wound epithelialisation following oral surgical procedures confirming photobiomodulation as an evidence-based adjunct for post-surgical wound healing acceleration. | Learning curve requirement for safe and effective laser use identified by a PRISMA-guided systematic review as the primary variable distinguishing successful from unsuccessful laser dental outcomes. Inadequate training and non-targeted device selection are the leading causes of laser treatment failures. |
Tokyo Medical and Dental University (TMDU) Laser-Assisted Pain Control After Periodontal Therapy: Systematic Review and Meta-Analysis, PMC7498060 | Manav Rachna Dental College, India Efficacy of Low-Level Laser Therapy on Oral Wound Healing: Systematic Review, PMC11531730, 2024 | MDPI Photonics Therapeutic and Adverse Effects of Lasers in Dentistry: Systematic Review (PRISMA), 2023 |
Vitrin Clinic Standard
Laser used where evidence supports it not everywhere
At Vitrin Clinic, laser treatment is selected for specific procedures where peer-reviewed evidence demonstrates measurable clinical advantage. It is not applied universally to every treatment as a marketing claim.
Wavelength and parameters matched to your procedure
The laser wavelength and energy settings used for each procedure are selected based on the tissue being treated and the clinical objective not a single default setting applied to every case.
Photobiomodulation offered after surgical procedures
Following soft tissue surgery, periodontal procedures, and implant placement, photobiomodulation is offered as a clinically evidence-supported adjunct for accelerating wound healing and reducing post-operative pain and swelling.
Reduced recovery for soft tissue procedures
Laser soft tissue surgery at Vitrin Clinic often eliminates the need for sutures, reduces post-operative swelling and pain, and accelerates healing compared to conventional scalpel techniques benefits directly confirmed in peer-reviewed clinical trials.
Clinical Evidence & References
Tokyo Medical and Dental University (TMDU), Japan
Patient-Reported Outcomes of Laser-Assisted Pain Control Following Non-Surgical and Surgical Periodontal Therapy Systematic Review and Meta-Analysis
PLOS ONE · September 2020Mikami R, Mizutani K, Iwata T, Aoki A et al. · DOI: 10.1371/journal.pone.0238659 · PMC7498060 · PubMed, Cochrane, Web of Science
Key finding: Adjunctive use of laser devices — both high-level (ablative) and photobiomodulation is significantly more effective at suppressing pain following periodontal therapy than conventional treatment alone, based on patient-reported outcome measures across included randomised controlled trials.
Manav Rachna Dental College, India
The Efficacy of Low-Level Laser Therapy on the Healing of Oral Wounds: A Systematic Review
Cureus · October 2024Gopal L, Palwankar P, Dhalla N · DOI: 10.7759/cureus.70832 · PMC11531730 · NLM, Google Scholar, Scopus · 14 RCTs included
Key finding: All 14 included studies found a substantial difference between laser and control groups in wound epithelialisation following oral surgical procedures. LLLT/PBM reduces inflammation, oedema, and post-surgical discomfort, and is preferred over conventional approaches specifically due to its healing capabilities and biostimulatory therapeutic profile.
First Affiliated Hospital of Zhengzhou University, China
The Clinical Efficacy of Laser in the Non-Surgical Treatment of Peri-Implantitis Systematic Review and Meta-Analysis
International Journal of Implant Dentistry · November 2024Huang N, Li Y, Li W et al. · DOI: 10.1186/s40729-024-00570-x · PMC11564455 · PubMed, Scopus, Cochrane, Web of Science
Key finding: Laser therapy used adjunctively to mechanical debridement produced clinical improvements in probing pocket depth and bleeding on probing in peri-implantitis cases demonstrating the bactericidal and anti-inflammatory benefits of laser irradiation in an environment where complete mechanical decontamination of implant surfaces is inherently challenging.
Frequently Asked Questions
Answers to common questions about the treatment, including suitability, procedure details, recovery, and long-term care — helping you feel informed and confident before moving forward.