Maintaining healthy gums is fundamental to long-term oral wellness. One of the most critical signs of advancing gum disease is the development of a periodontal pocket, a deepened gap between gum and tooth caused by bacterial infection and tissue damage. Understanding what these pockets are, why they form, and how they are treated can help you take timely action and protect your smile from irreversible harm and unnecessary tooth loss.
What Are Periodontal Pockets? Definition and Key Facts
Gum disease often begins silently, but its formation is one of its clearest clinical indicators. Recognizing the difference between healthy and diseased tissue, understanding key measurements, and knowing what pockets look like are essential steps toward better oral health awareness. This section defines what these pockets are, how they compare to a healthy gingival sulcus, and what depth readings mean for your overall gum health and long-term prognosis.
Periodontal Pocket Definition and Meaning
It describes a pathological deepening of the space between the tooth and surrounding gum tissue caused by infection and bone loss. In simple terms, it refers to a gap that traps bacteria and accelerates tissue destruction beneath the gumline. Clinically, any space measuring 4 mm or deeper is classified as a pocket, signaling the need for prompt professional evaluation and targeted treatment to prevent further irreversible damage.
Gingival Sulcus vs. Periodontal Pocket
Are related but distinctly different structures. A healthy gingival sulcus measures 1–3 mm and causes no harm. When bacterial infection leads to tissue detachment and bone destruction, this sulcus deepens into a true pathological space. Understanding this distinction helps patients grasp why elevated readings during dental probing should never be dismissed and why early intervention is critical for preserving gum tissue and preventing progressive bone loss around the tooth roots.
Normal and Abnormal Periodontal Pocket Depths
A normal periodontal pocket depth is one that is between 1 and 3 millimeters. Periodontal pockets 4mm signal early disease, while depths of 5–6 mm indicate moderate periodontitis. 8 mm pockets and 10 mm pockets represent severe disease with significant bone destruction. Tracking pocket depths over time is essential for assessing disease progression and determining whether non-surgical or surgical treatment is the most appropriate clinical approach for each individual patient.
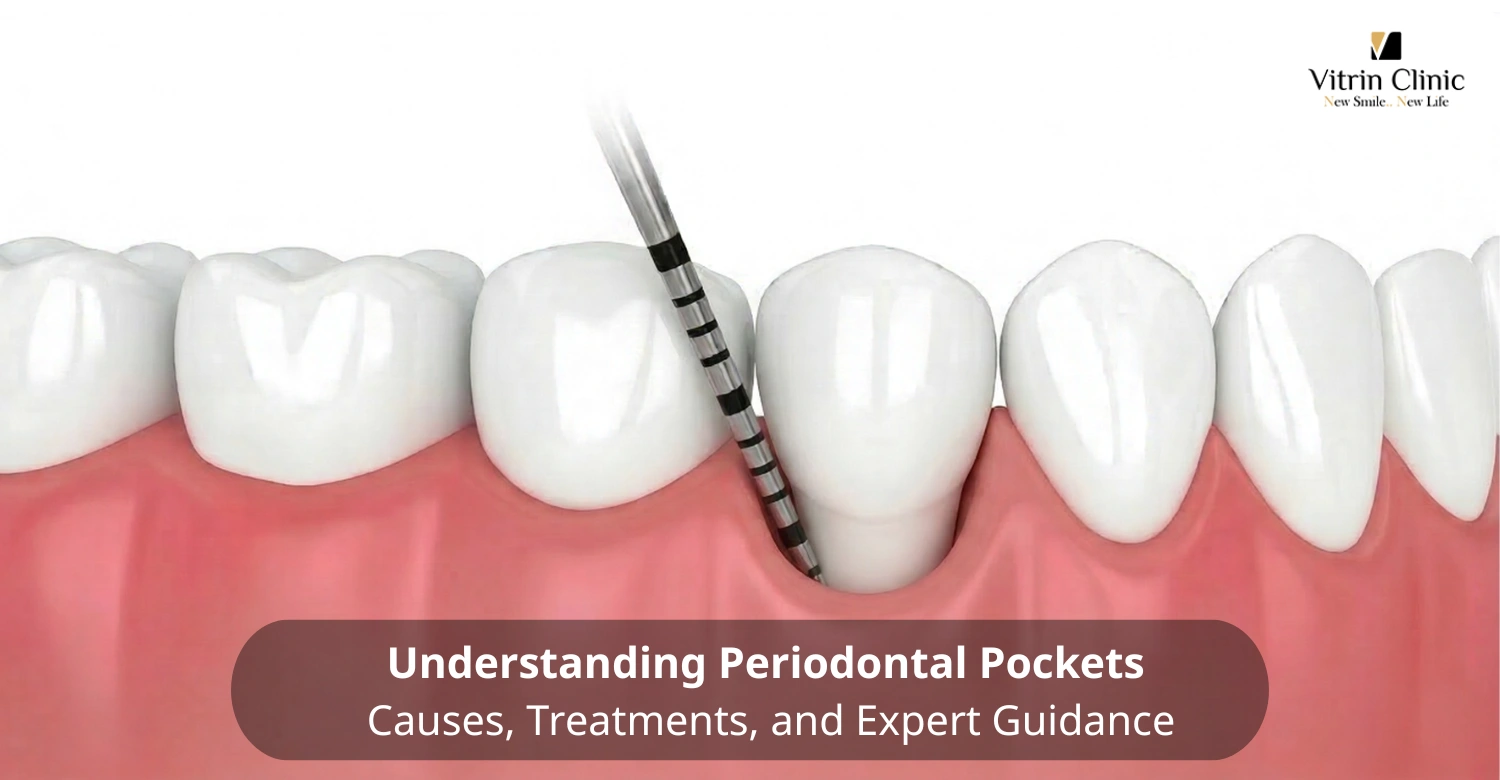
Visual Reference of Periodontal Pockets
Patients searching for periodontal pockets images want to understand what their condition looks like clinically. Affected gums typically appear red, swollen, and bleed easily during brushing or probing. Tissue pulls away from the tooth, creating visible gaps, and in advanced cases, exposed roots become apparent. Clinical photographs and X-rays taken during dental exams provide detailed visual references that help both clinician and patient monitor disease severity and evaluate treatment progress effectively.
Why Periodontal Pockets Develop
Understanding why these pathological spaces form is as important as knowing how to treat them. Multiple interconnected factors drive progression from healthy tissue to diseased pocketing. Periodontal pockets form due to causes that, when left unaddressed, lead to progressive destruction of gum and bone tissue. Identifying root causes and risk factors early allows for targeted intervention before significant bone loss occurs and before treatment options become more complex and costly for the patient.
Causes of Periodontal Pockets
It forms due to bacterial plaque accumulating along and beneath the gumline. When plaque is not consistently removed, it hardens into tartar, triggering chronic inflammation that destroys the connective tissue and bone supporting the teeth. Poor oral hygiene remains the primary driver, but aggressive bacterial strains and untreated gingivitis also contribute significantly. Left unmanaged, this cycle of infection and inflammation leads to progressive periodontal pocketing around multiple teeth over time.
Risk Factors for Deep Periodontal Pockets
Several factors increase vulnerability to deep gum pockets. Smoking significantly impairs blood flow and healing capacity, while diabetes, hormonal changes, genetic predisposition, stress, and dry-mouth-causing medications all heighten risk. Patients with these factors tend to develop more rapidly progressing periodontal gum pockets than the general population. Identifying individual risk factors during assessment allows clinicians to design more targeted prevention and treatment strategies that specifically address each patient’s unique clinical circumstances.
Progression from Mild to Severe Pockets
Gum disease progresses quietly. It typically begins with reversible gingivitis before advancing to early periodontitis with 4–5 mm readings. Without intervention, a 5 mm periodontal pocket can deepen to a 6 mm, then to 8 mm, and eventually to 10 mm. Each stage involves greater bone loss, increased tooth mobility, and a higher risk of permanent tooth loss underscoring why early professional cleaning and consistent monitoring are essential for preventing severe outcomes.
Patient Concerns and Common Problems
Many patients are alarmed when first diagnosed with periodontal gum pockets, particularly when they have experienced no significant pain. Symptoms can be subtle in early stages, making the condition easy to underestimate. However, untreated disease can have serious oral and systemic consequences. Understanding which symptoms to watch for and what complications arise from neglecting treatment helps patients make informed decisions and motivates them to seek timely, appropriate professional care before damage becomes irreversible.
Symptoms Associated with Periodontal Pockets
Common symptoms include persistent bad breath, red or swollen gums, bleeding during brushing, gum recession, tooth sensitivity, and loose teeth. Patients may also notice a bitter taste or visible changes in their gumline. A 6 mm periodontal pocket or deeper often causes noticeable discomfort during probing. Recognizing these warning signs early prompts patients to seek evaluation before the condition progresses to a stage where more invasive and costly treatment options become the only viable clinical solution available.
Complications of Untreated Deep Periodontal Pockets
When deep pockets go untreated, consequences extend well beyond the mouth. Progressive bone destruction leads to tooth loosening and eventual loss. Research also links advanced gum disease to cardiovascular conditions, diabetes complications, and respiratory infections. Patients requiring 9 mm periodontal pockets or 10 mm face complex, multi-step procedures that could have been avoided with earlier diagnosis and consistent professional care during the moderate stages of the disease.
Treatment Options
Effective periodontal pocket treatment depends on disease severity and the patient’s overall health. From conservative cleaning approaches to advanced surgical interventions, a range of evidence-based options exists to eliminate infection and restore healthy tissue. The goal of all treatment is to reduce depths, stabilize bone levels, and preserve natural teeth. This section outlines the full spectrum of available options, from non-surgical care through to advanced adjunctive therapies used for complex, severe cases.
Non-Surgical Treatments
Non-surgical care is the first line of defense for mild to moderate disease. Professional cleaning, antimicrobial rinses, and localized antibiotic therapy form the foundational approach. For pockets measuring up to 5–6 mm, these treatments can be highly effective. Patient compliance with home hygiene protocols directly impacts outcomes. Consistent follow-up appointments allow clinicians to monitor progress and determine whether meaningful periodontal pocket reduction has been achieved or whether escalation to more intensive treatment is clinically necessary.
Scaling and Root Planing for Deep Periodontal Pockets
Scaling and root planing effectiveness for deep pockets is well-documented in clinical research. This thorough procedure removes calculus and bacterial biofilm from below the gumline while smoothing root surfaces to discourage bacterial reattachment. It is especially effective for 8 mm periodontal treatment, often significantly reducing depths and inflammation. Scaling and root planing is frequently the foundational step before any decision is made regarding surgical intervention in more advanced cases.
Use of Periodontal Pocket Debridement Burs
It specialized rotary instruments used to remove calcified deposits and necrotic tissue from deep within infected pockets. These precision tools enhance cleaning of root surfaces and pocket walls beyond what manual instruments alone can achieve. They are particularly valuable when treating depths of 8 mm or greater, where standard scaler access is challenging. Incorporating debridement burs into treatment protocols improves root surface preparation and supports more predictable tissue healing outcomes.
Surgical Treatments for Severe Pockets
When non-surgical approaches are insufficient or depths exceed 6–7 mm, periodontal pocket surgery becomes necessary. Flap surgery provides direct access to root surfaces and bone, while osseous recontouring reshapes damaged bone architecture. For patients needing 9 mm periodontal treatment, surgery offers the most reliable long-term resolution. Bone grafting and guided tissue regeneration may also be incorporated into the surgical plan to rebuild lost structural support and improve the long-term prognosis of affected teeth.
Advanced and Adjunctive Therapies
Advanced adjunctive therapies increasingly complement standard treatment protocols. Laser-assisted therapy precisely removes infected tissue with minimal patient discomfort. Locally delivered antibiotics placed directly within pockets target resistant bacterial strains effectively. Photodynamic therapy and growth factor applications support tissue regeneration. These innovations enhance how to reduce periodontal pockets more effectively, particularly in complex or recurrent cases where conventional approaches alone have not fully resolved deep infections or where patients are unable to tolerate traditional surgical methods.
Benefits and Expected Outcomes of Treatment
Successfully completing treatment delivers measurable, lasting benefits beyond reduced depth readings. Patients experience healthier gum tissue, stabilized bone levels, reduced inflammation, and improved confidence in their smile. Understanding what to expect from periodontal pocket treatment helps set realistic goals and motivates continued commitment to care. Whether addressing mild or severe disease, the following sections outline the key clinical and quality-of-life improvements patients can realistically anticipate following comprehensive periodontal care.
Reduction in Periodontal Pocket Depths
A primary measurable outcome is significant reduction in periodontal pocket depth. Following scaling and root planing or surgery, depths typically decrease by 1–3 mm or more depending on initial severity. Patients presented with 8 mm periodontal pockets often achieve post-treatment readings of 3–4 mm, demonstrating successful infection elimination and tissue reattachment. Regular maintenance appointments help sustain these reductions and prevent recurrence of deeper, more destructive pocketing over time.
Improvements in Gum Health and Stability
Beyond reduced depths, treatment results in visibly healthier gums. Bleeding on probing decreases substantially, tissue color returns to a healthy pink, and chronic inflammation resolves. Patients notice reduced sensitivity and improved gum contour around their teeth. Stabilizing periodontal gum pockets prevents further bone loss and creates a favorable environment for long-term maintenance. These improvements are clinically measurable and highly noticeable to patients in their day-to-day oral health experience.
Long-Term Oral Health Benefits
Treating deep pockets has lasting benefits for both oral and systemic health. Reduced bacterial load lowers inflammation linked to cardiovascular disease and diabetes. Preserved bone levels support natural teeth for decades. Patients who learn how to heal periodontal pockets through consistent home care and professional monitoring enjoy significantly better overall health outcomes. Long-term success requires ongoing maintenance, as gum disease can reactivate without proper follow-up care and routine professional cleaning to sustain treatment gains.
Preventive Advice and Daily Dental Care
Prevention remains the most powerful tool against gum disease. Strong daily hygiene habits and consistent professional care significantly reduce the risk of developing or worsening periodontal pockets. Patients who understand how their lifestyle choices affect gum health are better equipped to protect themselves long-term. The following guidance covers proven home care strategies and professional recommendations designed to keep depths within the healthy range and prevent progression to more serious stages of destructive periodontal disease.
Home Care to Maintain Healthy Gums
Learning how to get rid of periodontal pockets starts with consistent daily habits. Brushing twice daily with a soft-bristled toothbrush, flossing every day, and using an antimicrobial rinse are foundational practices. Interdental brushes and water flossers help clean effectively between teeth and below the gumline. These habits complement professional treatment and directly influence healing speed. Patients who master effective home care techniques play an active role in reducing their risk of recurrent or worsening gum disease.
Regular Professional Checkups
Routine dental visits every three to six months are essential for managing and preventing gum disease. During these appointments, clinicians measure depths, perform professional cleaning, and assess home care compliance. Early detection of any new pocketing allows timely treatment adjustments before disease progresses significantly. Patients with a history of periodontitis are strongly advised to maintain more frequent recall appointments, as periodontal pocketing can reactivate even after prior successful treatment without ongoing professional monitoring and cleaning.
Lifestyle and Habits to Prevent Periodontal Pockets
Lifestyle choices directly influence gum health outcomes. Quitting smoking dramatically reduces risk and improves treatment response. Managing conditions like diabetes helps regulate immune function and systemic inflammation. A nutrient-rich diet supports gum tissue integrity, while stress management lowers inflammatory markers in the body. Staying well-hydrated prevents dry mouth, which accelerates bacterial growth along the gumline. Collectively, these habits form a comprehensive prevention strategy that reduces the likelihood of developing deep, destructive gum pockets over time.
Patient Education and Professional Guidance
Empowering patients with accurate, easy-to-understand information leads to better treatment compliance and long-term outcomes. Many patients arrive anxious about their diagnosis and uncertain about what lies ahead. Clear communication, individualized guidance, and a collaborative approach between clinician and patient are essential components of successful care. This section addresses common patient questions and explains how personalized treatment planning sets clear expectations, reducing anxiety while ensuring each patient receives care tailored specifically to them.
Common Questions About Periodontal Pockets
Patients frequently ask what are periodontal pockets, how they are measured, whether they cause pain, and what happens if left untreated. Others want to know how to shrink periodontal pockets at home or whether their case requires surgery. Providing clear, direct answers to these questions during consultations builds trust and reduces anxiety. Addressing the full range of depth measurements and their clinical implications helps patients feel informed, confident, and genuinely motivated to commit to their recommended treatment plan.
Personalized Treatment Planning and Expectations
No two cases of gum disease are identical. Personalized planning considers depth readings, systemic health, smoking history, lifestyle, and compliance capability. Some patients with moderate 6 mm pockets may need only non-surgical care, while those with deeper readings require surgical intervention. Setting realistic expectations about healing timelines, discomfort levels, and required maintenance visits ensures patients enter care fully prepared. A thorough initial assessment is the cornerstone of designing a treatment pathway that achieves lasting, predictable gum health improvements.
Vitrin Clinic Expertise in Periodontal Care
At Vitrin Clinic, gum care is delivered with the highest standards of clinical excellence. Whether you are dealing with early-stage pockets or require complex surgical intervention, our team is fully equipped to provide comprehensive, compassionate treatment. Combining advanced technology, extensive expertise, and a genuinely patient-centered approach, Vitrin Clinic delivers outstanding outcomes for both local residents and international patients who travel to Istanbul for world-class dental treatment at highly competitive prices.
Advanced Technology and Techniques
Vitrin Clinic utilizes state-of-the-art diagnostic and treatment tools to ensure precision gum disease management. Digital periodontal charting allows real-time tracking of depth readings across multiple visits. Laser-assisted therapy, ultrasonic scalers, and specialized debridement instruments enable thorough cleaning even in the most challenging deep cases. These advanced technologies improve diagnostic accuracy, reduce patient discomfort, and enhance treatment outcomes helping patients achieve meaningful depth reductions in fewer appointments compared to conventional treatment approaches.
Experienced Dentists for Periodontal Pocket Reduction
The dental professionals at Vitrin Clinic bring extensive experience in managing all stages of gum disease, from early 4 mm readings to complex 10 mm cases requiring surgical intervention. Each clinician applies evidence-based protocols, combining expertise with the latest periodontology research. Patients receive personalized care from a team that understands both the clinical complexity and the emotional impact of being diagnosed with deep gum disease, ensuring a supportive, thorough experience from first appointment through long-term maintenance.
Comprehensive Care for Local and International Patients
Vitrin Clinic warmly welcomes both local and international patients seeking high-quality gum disease treatment in Istanbul. Our multilingual team ensures seamless communication and comfort throughout the entire treatment journey. From initial consultation and professional cleaning through to surgical care and ongoing follow-up, every step is carefully coordinated to ensure a smooth, stress-free experience. International patients benefit from competitive pricing, comprehensive treatment planning, and a dedicated support team assisting with travel, accommodation, and post-treatment care guidance.
Book a FREE Consultation At Vitrin Clinic
If you have been diagnosed with deep gum pockets, are experiencing symptoms of gum disease, or simply want to understand your depth readings better, now is the ideal time to take action. Vitrin Clinic offers a FREE consultation to thoroughly assess your gum health, explain all available options, and create a personalized treatment plan tailored to your specific needs. Take the first step toward a healthier, stronger smile.. book your FREE consultation with Vitrin Clinic in Istanbul today.
FAQs
What is a periodontal pocket and how is it measured?
Is a pathological space that forms between the tooth and gum when bacterial infection causes tissue detachment and bone loss. It is measured using a calibrated probe inserted gently along the gumline at multiple points around each tooth. Healthy readings are 1–3 mm. Depths of 4 mm and above indicate disease, while 6 mm or deeper signals moderate to severe gum disease requiring professional evaluation and a targeted, personalized treatment plan.
What do 8 mm periodontal pockets indicate?
8 mm periodontal pockets indicate advanced periodontitis with significant bone loss and extensive tissue destruction. At this depth, bacteria thrive in an environment extremely difficult to clean with standard instruments. 8 mm pockets typically begin with scaling and root planing, often followed by surgical intervention for full resolution. Without treatment, this level of pocketing will continue to progress, increasing tooth mobility and substantially raising the long-term risk of permanent tooth loss.
Can deep periodontal pockets lead to tooth loss?
Yes, deep pockets are among the leading causes of adult tooth loss worldwide. As infection progresses, it destroys the bone and connective tissue anchoring the teeth, causing them to loosen gradually over time. Without timely treatment, affected teeth may eventually require extraction. Seeking professional care promptly for depths of 6 mm or greater significantly reduces tooth loss risk. Effective treatment combined with strong daily home care can successfully halt disease progression and preserve natural dentition long-term.
How to shrink periodontal pockets effectively?
It involves professional treatment combined with rigorous daily oral hygiene. Scaling and root planing works well for moderate cases, while surgery is required for deeper disease. Consistent brushing, flossing, and antimicrobial rinsing support clinical outcomes at home. Patients who commit to regular professional cleanings, follow post-treatment guidance, and make positive lifestyle changes, particularly quitting smoking, achieve the greatest long-term results in reducing and stabilizing their gum pocket depths.
Treatment options for 10 mm periodontal pockets?
Typically requires surgical intervention due to extreme depth and substantial bone loss. Flap surgery, osseous recontouring, bone grafting, and guided tissue regeneration are all common procedures at this stage. Post-surgical care includes antimicrobial therapy and frequent follow-up monitoring. Despite the severity, these cases can be successfully managed with experienced clinicians and strong patient compliance. Early action remains the best strategy for preventing pockets from ever reaching this advanced and clinically complex stage.
Can periodontal pockets be reversed?
Whether pockets can be reversed depends heavily on severity. Early-stage disease with proper treatment and improved hygiene can lead to significant tissue reattachment and depth reduction. However, bone loss associated with deeper disease is generally not fully reversible without regenerative surgical procedures. This question is best answered during a comprehensive clinical evaluation, where a specialist assesses current depth readings, bone levels, and tissue quality to determine the most realistic and appropriate treatment pathway available.
How effective is scaling and root planing for deep pockets?
Scaling and root planing effectiveness for deep pockets is well-supported by clinical evidence. Studies consistently show depth reductions of 1–3 mm following the procedure, especially in pockets measuring 5–7 mm. For 8 mm cases, it serves as a critical initial step that often reduces inflammation enough to evaluate whether surgery is still needed afterward. Patient compliance with post-treatment hygiene protocols and maintenance visit frequency significantly influences how durable and long-lasting the clinical outcomes will be.
How to maintain healthy gums and prevent periodontal pockets?
How to get rid of periodontal pockets and prevent their recurrence requires combining daily oral care with consistent professional monitoring. Brush twice daily, floss regularly, and use antimicrobial rinses to minimize bacterial load. Attend professional cleanings every three to six months and seek prompt evaluation of any readings above 3 mm. Quit smoking, manage chronic health conditions, and follow a balanced diet. These combined habits form the most reliable foundation for preventing gum disease and maintaining lasting oral wellness.