Endodontics
- Home
- Treatments
- Endodontics
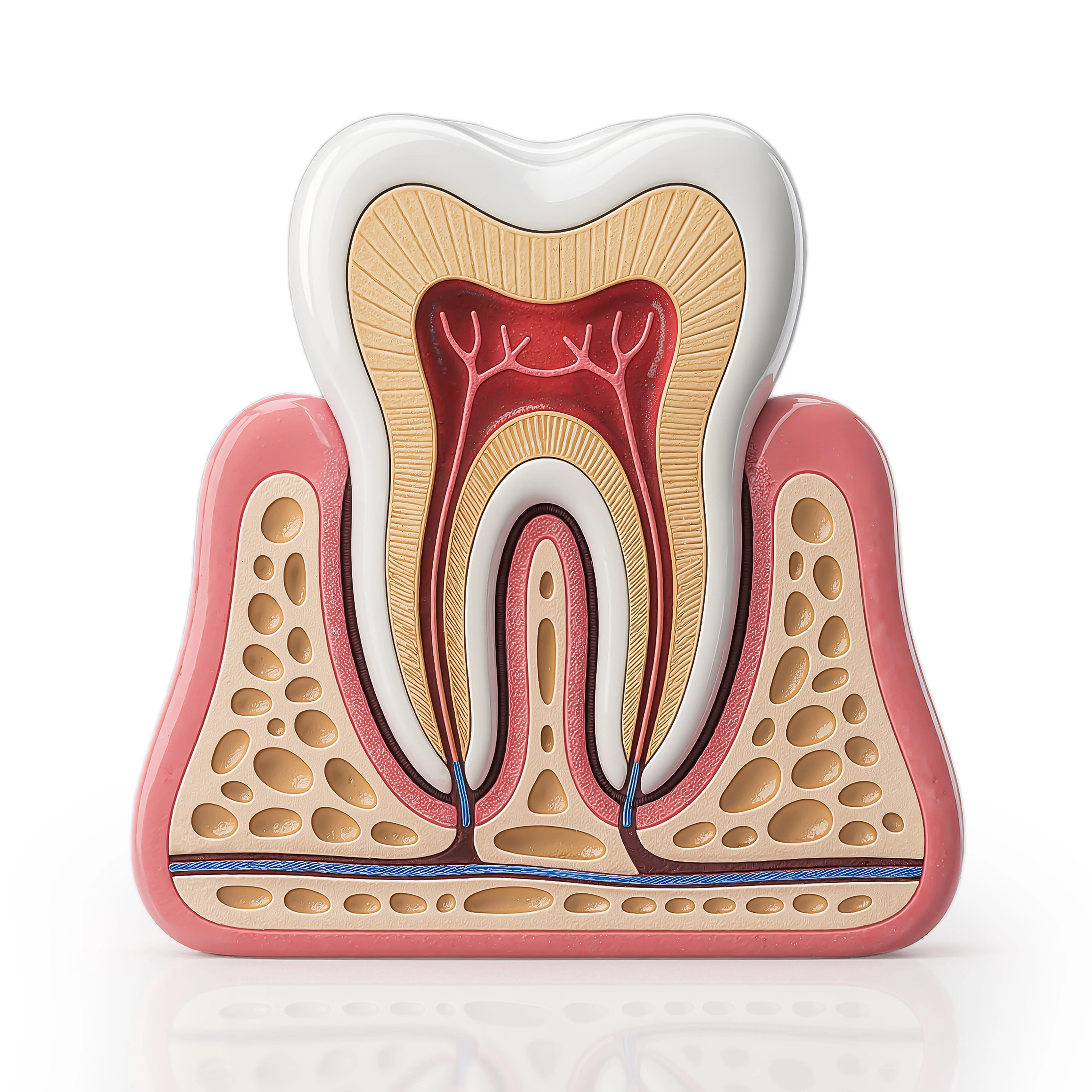
Endodontic therapy in Turkey has evolved dramatically. At Vitrin Clinic we combine rotary endodontics, laser endodontic treatment, apex locators, and digital X-rays to make every procedure faster, safer, and virtually pain-free.
Treatment Process
A clear step-by-step overview of how the treatment is planned and performed, from the initial consultation to the final results, ensuring comfort, safety, and predictable outcomes.
01
Diagnosis & Digital Imaging
We begin with a comprehensive clinical examination and digital X-rays or CBCT 3D scan. This reveals the number of canals, root anatomy, infection extent, and surrounding bone condition giving us the full picture before we begin.
02
Anaesthesia & Isolation
Local anaesthesia is administered to ensure complete comfort throughout the procedure. A rubber dam is placed to isolate the tooth, maintaining a sterile field and protecting you from irrigating solutions.
03
Canal Access & Pulp Removal
A small access cavity is created through the crown. Our specialist uses ultrasonic instruments and magnification loupes to locate all canals and fully remove infected or necrotic pulp tissue.
04
Shaping, Cleaning & Laser Disinfection
Rotary nickel-titanium files guided by an electronic apex locator clean and shape the canals to their precise working length. Sodium hypochlorite irrigation and laser endodontic treatment then eliminate any remaining bacteria deep within the dentinal tubules.
05
Canal Obturation
The cleaned canals are filled and sealed with biocompatible gutta-percha using warm vertical condensation the gold standard technique preventing any future bacterial re-entry.
06
Restoration & Crown Placement
A root-canal-treated tooth is more brittle and requires protection. We restore the access cavity and, in most cases, recommend a porcelain crown to restore full strength, function, and aesthetics.
What Is Endodontic Treatment?
Endodontics is the branch of dentistry concerned with the diagnosis and treatment of diseases affecting the dental pulp the soft tissue at the centre of a tooth containing nerves, blood vessels, and connective tissue.
When the pulp becomes irreversibly inflamed or infected, it cannot heal on its own.
Without treatment, the infection progresses through the root canal system into the surrounding bone, producing an abscess and ultimately threatening the tooth's survival.
The primary objective of endodontic treatment is to eliminate infection, prevent reinfection, and preserve the natural tooth in function for as long as possible.
Root canal treatment the most common endodontic procedure involves the removal of the diseased pulp tissue, thorough cleaning and shaping of the root canal system, disinfection, and three-dimensional obturation to seal the canals against bacterial recontamination.
The tooth is then restored with a post-and-core buildup where required and a definitive coronal restoration typically a full ceramic crown for posterior teeth to protect the remaining tooth structure and restore function.
85–97%Success Rate (Vital Teeth) | 37yrLongest Documented Follow-Up | 1–2Appointments Typically | 3DCanal Obturation Standard |
|---|---|---|---|
When Is Endodontic Treatment Indicated?
Endodontic treatment is indicated when the dental pulp has been irreversibly damaged — either through bacterial invasion from deep decay, traumatic injury, or prolonged pulpal inflammation that has exceeded the tissue's capacity for repair. Symptoms vary from acute pain and swelling to no symptoms at all, which is why diagnosis requires clinical examination combined with radiographic assessment rather than symptom severity alone.
Irreversible Pulpitis
Irreversible pulpitis is the clinical diagnosis made when pulp inflammation has progressed beyond the point of spontaneous resolution. It is characterised by persistent, lingering pain in response to thermal stimuli particularly cold that continues for 30 seconds or more after the stimulus is removed. At this stage, the pulp cannot recover regardless of the cause being addressed, and root canal treatment is the only tooth-preserving intervention available.
Pulp Necrosis & Apical Periodontitis
Pulp necrosis death of the pulp tissue may develop silently following untreated pulpitis, trauma, or the progression of deep decay. The necrotic pulp becomes a reservoir for bacterial colonisation, leading to apical periodontitis infection of the bone surrounding the root tip. Radiographically, this appears as a periapical radiolucency: a dark shadow at the root apex indicating bone destruction from the spreading infection. Root canal treatment is indicated to eliminate the bacterial load and allow periapical bone healing.
Dental Trauma with Pulpal Involvement
Traumatic injuries crown fractures exposing the pulp, luxation injuries, or avulsions can compromise pulpal vitality acutely or over time. Where pulpal exposure or loss of vitality is confirmed following trauma, endodontic treatment is indicated to prevent bacterial colonisation of the root canal system and periapical infection. In cases of dental avulsion or intrusive luxation, the decision and timing of endodontic treatment requires careful clinical judgement based on root maturity, extraoral dry time, and storage medium.
Pre-Prosthetic Endodontics
In some cases, endodontic treatment is performed on teeth that have not yet developed symptomatic pulpitis but whose crown destruction or existing restorations make future pulp exposure likely during preparation for a crown or post-supported restoration. This is a planned, preventive indication performed to ensure the tooth can support the planned restoration without the risk of post-operative symptoms or emergency re-entry through a completed crown. Each case is evaluated carefully against the risks of elective pulp removal.
Failed or Inadequate Previous Root Canal
Persistent or recurrent periapical pathology following root canal treatment may indicate an incompletely obturated canal system, missed canals, canal transportation, or coronal microleakage contaminating a previously adequate obturation. Non-surgical re-treatment retreating through the existing restoration and filling is the first-line approach. Systematic review data reports success rates of 71 to 87% for non-surgical retreatment over 1 to 3 years, with periapical lesion size and initial PAI score as the primary prognostic factors.
Save the Tooth First
The international endodontic evidence base consistently supports tooth preservation as the primary clinical objective wherever it is achievable. A 2025 systematic review comparing endodontically treated teeth and implant-supported prostheses published in PMC/NIH concluded that both modalities have excellent survival rates, but that saving a natural tooth through root canal treatment should be the preferred first-line approach. The natural tooth root maintains alveolar bone, preserves proprioception, and eliminates the biological and surgical risks associated with implant placement. Extraction is irreversible. Root canal treatment is not.
Root Canal Treatment vs. Extraction and Replacement
When a tooth requires endodontic treatment, patients are sometimes presented with extraction as an alternative.
The following comparison is based on peer-reviewed clinical evidence and outcome data from prospective controlled cohort studies and systematic reviews.
Criterion | Root Canal Treatment | Extraction + Implant | Extraction + Bridge | Extraction Only |
|---|---|---|---|---|
Preserves Natural Tooth | Yes, tooth root and periodontal ligament retained | No , natural tooth lost permanently | No, adjacent teeth also prepared | No, space left unrestored |
Alveolar Bone Preservation | Yes, root stimulates bone; no resorption | Partial - implant stimulates bone but no PDL | No, bone resorption continues beneath pontic | No, significant bone loss follows extraction |
Proprioception (Tactile Feedback) | Maintained - periodontal ligament intact | Lost - implant osseointegrates without PDL | Lost at extracted site | Lost |
Treatment Invasiveness | Non-surgical - no incision or bone involvement | Surgical - extraction, potential grafting, implant surgery | Extraction + preparation of adjacent teeth | Surgical extraction only |
Overall Treatment Duration | 1–2 appointments to completion | 3–9 months including osseointegration | 2–3 weeks for conventional bridge | Single appointment |
Long-Term Survival | 85–97% success (vital teeth); 5–37yr follow-up documented | >95% at 10 years comparable long-term data | ~89% at 10 years - abutment tooth risk | Permanent tooth loss with downstream consequences |
Adjacent Teeth Affected | None - treatment isolated to the affected tooth | None - implant is standalone | Yes, adjacent teeth prepared and permanently altered | Adjacent teeth may drift over time |
Quality of Life Impact | Significant improvement - University of Gothenburg prospective cohort, 12-month follow-up | High satisfaction - but longer treatment timeline | Good - restoration of function | Reduced - functional and aesthetic deficit persists |
Compiled from: University of Gothenburg (Sahlgrenska Academy) RCT vs. Extraction: Quality of Life Prospective Cohort, PMC11487112, 2024 · University of Gothenburg Cost-Effectiveness of RCT vs. Extraction, PMC10441609, 2023 · NIH/PMC Comparative Outcomes of Endodontically Treated Teeth vs. Implants, PMC12239130, 2025 · UCL Eastman Dental Institute Outcomes of Primary RCT Systematic Review.
Why Clinical Approach Matters
The success rate of root canal treatment varies considerably in the peer-reviewed literature from 68% to 97% depending on the study and this variation is not random.
It is explained by three consistently identified clinical variables: the pre-operative periapical status of the tooth, the technical quality of canal preparation and obturation, and the integrity of the coronal restoration placed after treatment.
All three are directly determined by clinical decision-making and technical execution, not by the patient.
The most significant single predictor of endodontic success is the pre-operative periapical status.
Teeth treated before periapical pathology develops at the stage of irreversible pulpitis with a vital pulp consistently achieve higher success rates than teeth with established periapical lesions.
This makes early diagnosis and timely treatment the highest-value clinical intervention in endodontics.
A tooth treated while the pulp is still vital has a fundamentally better prognosis than one treated months later after necrosis and periapical infection have developed.
The coronal restoration is equally critical. A 2025 systematic review on root canal filling techniques and outcomes published in PMC/NIH confirmed that the quality of the final coronal seal is as important as the quality of the obturation itself.
A perfectly cleaned and obturated canal system contaminated by coronal microleakage through an inadequate restoration will fail regardless of the endodontic quality.
At Vitrin Clinic, restoration planning begins at the endodontic assessment appointment, not after treatment is completed.
What the research shows
85–97% | Equivalent | Cost-Effective | |
|---|---|---|---|
Success rate for root canal treatment of vital teeth (irreversible pulpitis, no periapical pathology) using contemporary protocols the highest recorded endodontic success category. Success rates are lower for teeth with pre-existing periapical lesions, confirming the value of early treatment. | Long-term survival rates between endodontically treated teeth and implant-supported prostheses confirming that root canal treatment is a clinically comparable alternative to implant replacement for suitable teeth, with the additional benefit of preserving the natural tooth root and alveolar bone. | Root canal treatment compared favourably to extraction on cost-effectiveness analysis measured in cost per quality-adjusted life year (QALY) gained in a prospective controlled cohort study from the University of Gothenburg, confirming that tooth preservation is both clinically and economically the more efficient approach where the tooth is restorable. | |
NIH/PMC Outcomes of Primary Root Canal Therapy 2003–2020 Systematic Review, PMC9322405 · University Complutense of Madrid Long-Term Survival 5–37 Years, PMC10264502 | NIH/PMC Comparative Outcomes of Endodontically Treated Teeth vs. Dental Implants, PMC12239130, 2025 | University of Gothenburg (Sahlgrenska Academy) Cost-Effectiveness of RCT vs. Extraction, PMC10441609, 2023 |
Vitrin Clinic Standard
Diagnosis before treatment every time
Root canal treatment is performed only where the clinical and radiographic diagnosis confirms it is indicated. The treatment follows the diagnosis not the other way around.
Rubber dam is mandatory no exceptions
Every root canal procedure at Vitrin Clinic is performed under rubber dam isolation. Saliva contamination during treatment is a direct cause of endodontic failure and it is fully preventable.
Obturation verified before sealing
A radiograph confirming the quality of obturation is taken before the tooth is sealed and the patient leaves the chair. Inadequate obturation is corrected at the time of treatment not discovered at a recall appointment.
Crown planned from the start
The definitive coronal restoration is discussed and planned at the initial assessment so the endodontic treatment and the crown are managed as a unified sequence, not as two separate decisions made months apart.
Clinical Evidence & References
NIH / PubMed Central Updated Systematic Review
Outcomes of Primary Root Canal Therapy Updated Systematic Review of Longitudinal Clinical Studies Published 2003–2020
International Endodontic Journal · July 2022PubMed, Embase, CINHAL, Cochrane, Web of Science · PMC9322405 · DOI: 10.1111/iej.13664
Key finding: Contemporary root canal treatment achieves favourable healing outcomes. Pre-operative periapical status is the strongest predictor of success teeth treated without periapical pathology (vital pulp cases) consistently achieve higher success rates than teeth with established lesions, confirming the clinical value of early diagnosis and treatment.
UCL Eastman Dental Institute, University College London, UK
Outcome of Primary Root Canal Treatment Systematic Review of the Literature, Part I: Effects of Study Characteristics on Probability of Success
International Endodontic Journal · 2007–2008Ng YL, Mann V, Rahbaran S, Lewsey J, Gulabivala K · PubMed PMID: 17931389 · MEDLINE and Cochrane 1966–2002
Key finding: Pooled success rates of primary root canal treatment ranged between 68% and 85% under strict criteria with the wide range explained by pre-operative periapical status, quality of obturation, and coronal seal integrity. This landmark review established the three primary determinants of endodontic success that remain central to clinical decision-making today.
University of Gothenburg, Sahlgrenska Academy, Sweden
A Comparison of Oral Health-Related Quality of Life and Satisfaction Among Patients Undergoing Root Canal Treatment or Tooth Extraction Prospective Controlled Cohort Study
Acta Odontologica Scandinavica · October 2024Wigsten E, Camci E, Levinsson A, Kvist T et al. · DOI: 10.2340/aos.v83.42011 · PMC11487112
Key finding: Root canal treatment produced significant improvements in oral health-related quality of life measured by OHIP-14 across 1, 6, and 12-month follow-up, with high patient satisfaction scores. Quality of life improvement was comparable between root canal treatment and tooth extraction groups, supporting tooth preservation as the clinically and patient-centred preferred approach.
University of Gothenburg & Linköping University, Sweden
Cost-Effectiveness of Root Canal Treatment Compared with Tooth Extraction in a Swedish Public Dental Service Prospective Controlled Cohort Study
Clinical and Experimental Dental Research · June 2023Wigsten E, Kvist T, Husberg M, Davidson T · DOI: 10.1002/cre2.759 · PMC10441609
Key finding: Root canal treatment compared favourably to extraction in cost-effectiveness analysis measured in cost per quality-adjusted life year (QALY) gained confirming that preserving a natural tooth through root canal treatment is both clinically effective and economically efficient in a general dental practice setting.
NIH / PubMed Central Systematic Review
Comparative Outcomes of Endodontically Treated Teeth Versus Dental Implant-Supported Prostheses Systematic Review
NIH/PMC · 2025Six databases: Cochrane, Embase, Medline, LILACS, Scopus, Web of Science · PMC12239130
Key finding: Both root canal therapy and dental implants demonstrate excellent long-term survival rates. Saving the natural tooth through root canal treatment should be the preferred first-line approach where the tooth is restorable preserving alveolar bone, periodontal ligament proprioception, and avoiding the biological and surgical risks associated with extraction and implant placement.
University Complutense of Madrid, Spain
Long-Term Tooth Survival and Success Following Primary Root Canal Treatment 5 to 37-Year Retrospective Observation
Clinical Oral Investigations · March 2023López-Valverde I, Vignoletti F, Martin C, Sanz M · DOI: 10.1007/s00784-023-04938-y · PMC10264502
Key finding: Long-term retrospective observation over 5 to 37 years confirms that primary non-surgical root canal treatment achieves clinically meaningful tooth retention over decades when combined with adequate coronal restoration with tooth survival rates among the highest reported in long-term endodontic literature.
NIH / PubMed Central Systematic Review & Meta-Analysis
Effect of Root Canal Filling Techniques and Materials on Endodontic Treatment Outcomes
Scientific Reports · 2026PubMed, Cochrane, ScienceDirect · PRISMA-guided · PMC13009500 · ≥6 months follow-up
Key finding: The quality of both obturation and coronal restoration are primary determinants of endodontic success findings consistent across obturation techniques and materials. Coronal microleakage from inadequate restoration contaminates a technically satisfactory obturation and represents one of the most significant causes of post-treatment failure.
NIH / PubMed Central Clinical Outcomes Review
Endodontic and Dental Implant Treatment: Key Considerations and Comparisons
NIH/PMC · 2025Includes British Dental Journal Dental Practicality Index · PMC12101971
Key finding: Both endodontic treatment and implants have excellent survival rates, but neither is a universal solution. Holistic, evidence-based treatment planning using structured assessment tools including the Dental Practicality Index is required to determine the appropriate intervention for each individual tooth based on endodontic need, periodontal status, structural integrity, and clinical context.
Frequently Asked Questions
Answers to common questions about the treatment, including suitability, procedure details, recovery, and long-term care — helping you feel informed and confident before moving forward.
.webp&w=3840&q=75)



.webp&w=3840&q=75)



.webp&w=3840&q=75)
.webp&w=3840&q=75)
.webp&w=3840&q=75)
